Can you imagine a topical treatment that targets the hormonal cause of androgenetic alopecia, but with minimal systemic exposure? For years, the therapeutic “menu” for androgenetic alopecia (AGA)—pattern hair loss—has relied mainly on two pillars: blocking androgen action with 5-alpha-reductase inhibitors (finasteride/dutasteride) and stimulating the follicle with minoxidil. They work, yes, but they’re not perfect: they require consistency, can cause side effects, and not everyone feels comfortable with oral medication.
In this context, clascoterone 5% emerges—a topical drug with a different approach: it doesn’t aim to lower DHT levels in the bloodstream, but rather to block the androgen receptor locally in the scalp. That makes it one of the most interesting developments of recent years.
What is androgenetic alopecia?
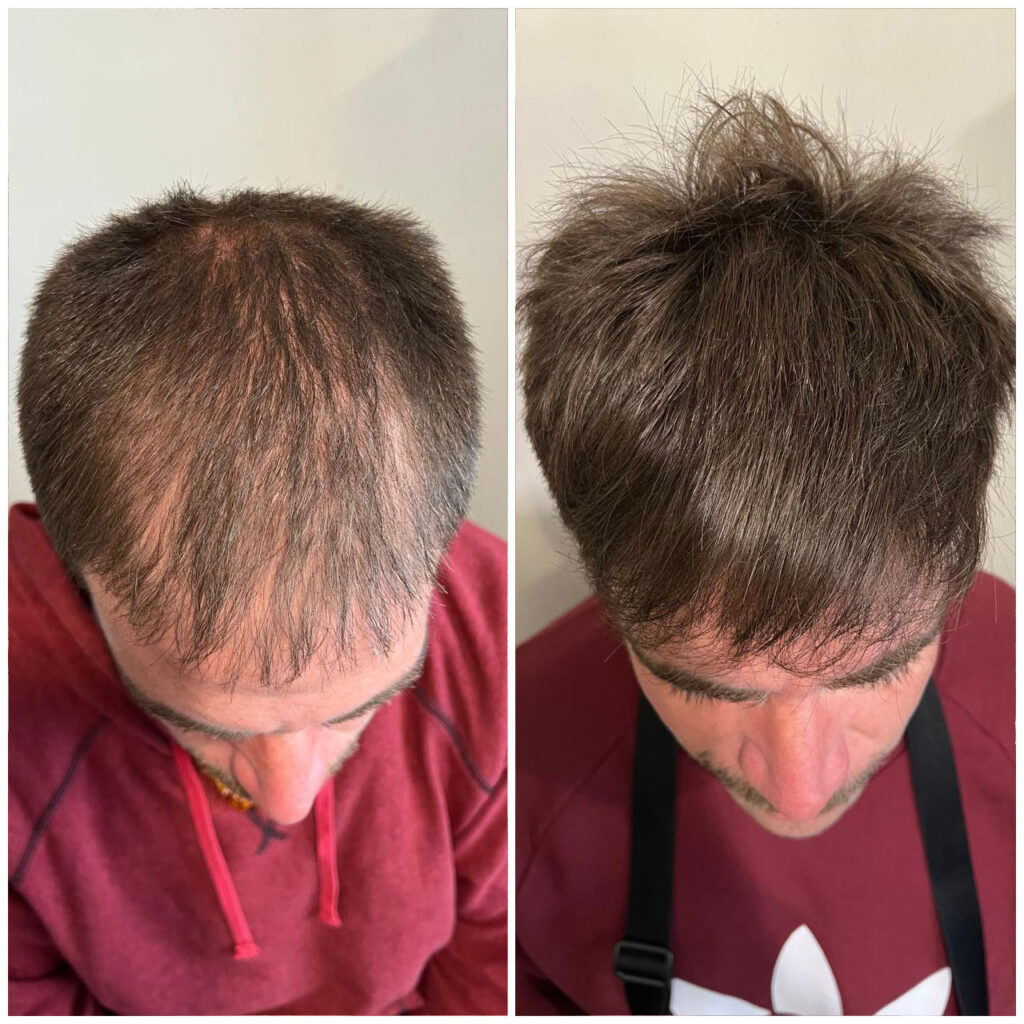
AGA is the most common form of hair loss in both men and women. It’s not a uniform “shedding”: it’s a progressive process in which the follicle gradually miniaturizes. With each cycle, the hair tends to grow thinner, shorter, and with less pigment, until visible density decreases.
The role of DHT in follicular miniaturization
Dihydrotestosterone (DHT)—a derivative of testosterone produced by the enzyme 5-alpha-reductase—binds to the androgen receptor in follicular structures. In genetically predisposed individuals, this androgen signal:
- shortens the anagen phase (growth),
- prolongs or favors resting phases,
- reduces hair shaft diameter,
- and causes the affected area to lose density over time.
That’s why early diagnosis improves the chances of slowing the process and preserving viable follicles.
Current treatments and their limitations
1) 5-alpha-reductase inhibitors (finasteride/dutasteride)
These are oral medications that reduce the conversion of testosterone into DHT. In many patients, they help stabilize the condition and, in some cases, partially restore density. The issue is that, because they act systemically, some people:
- fear sexual or mood-related side effects,
- don’t want long-term oral medication,
- or discontinue them due to tolerance or personal preference.
2) Minoxidil (topical or oral in certain cases)
Minoxidil is a follicle stimulant. It can help thicken hair and sustain growth, but it requires consistency, and once discontinued, the gains tend to gradually disappear. Additionally, some people experience scalp irritation with topical formulations or don’t tolerate certain presentations.
The therapeutic “gap”
In simple terms: there has been a lack of a topical option with a direct antiandrogen mechanism, designed for people who don’t want or can’t use oral medication. That’s where clascoterone could add value.
What is clascoterone?
Clascoterone is a topical androgen receptor inhibitor. Its core idea is simple:
- DHT may be present.
- But if it cannot activate the receptor in the follicle, its biological effect is reduced.
How is it different from finasteride/dutasteride?
- Finasteride/dutasteride: reduce DHT (via 5-alpha-reductase), with systemic impact.
- Clascoterone: targets the local androgen receptor, aiming to minimize systemic absorption.
A relevant dermatological safety note
The active ingredient is already used in dermatology in acne formulations (in other markets), which provides some background on skin tolerability. This does not mean it is already approved for alopecia: it means the ingredient is known in dermatology and is being adapted for a new therapeutic target.
Phase 3 clinical trial results: what is known so far
The most cited pivotal phase 3 studies are SCALP 1 and SCALP 2, involving a total of 1,465 adult men with androgenetic alopecia. In publicly shared preliminary results:
- one trial showed a marked relative improvement in hair count in the target area,
- the other also showed significant improvement, although of smaller relative magnitude,
- and the adverse event profile reported was generally comparable to the vehicle (placebo).
How to interpret these numbers without exaggeration
It’s important to translate this into clinical language:
- Los “porcentajes relativos” suenan enormes, pero lo relevante para el paciente es:
- whether there is real, measurable improvement (density, thickness),
- whether that improvement is visible and sustained,
- and what the long-term tolerability and adherence look like.
In alopecia, the initial goal is often not “going back to 18,” but rather slowing progression, restoring some thickness, and improving the facial frame with a natural result.
Advantages over oral treatments
The main promise of clascoterone is its local action. What could that imply if confirmed and approved?
It may be an option for those who avoid systemic treatments.
It could be used in combination regimens, under medical guidance, with:
- minoxidil,
- supportive therapies (e.g.,
- regenerative approaches),
- and post-transplant maintenance strategies.
Additionally, for some patient profiles, a topical antiandrogen option may improve adherence: when a treatment plan is easier to maintain, results tend to be more consistent.
Who could benefit?
Without replacing medical evaluation, the “logical” profiles where it might fit (if approved and adopted) include:
- men with mild to moderate AGA seeking a topical alternative,
- patients who do not tolerate or do not want oral medication,
- cases where a local antiandrogen is part of a combined approach,
- individuals in post-transplant maintenance to protect native hair (per medical indication).
What about women?
Female androgenetic alopecia exists and is common, but any hormonal treatment requires individualized evaluation, including medical history, age, reproductive status, and risk profile. In general, topical options tend to be better accepted, but specific indications depend on approval, targeted evidence, and clinical context.
Regulatory outlook and availability
Clascoterone for androgenetic alopecia still depends on:
- complete data (including longer-term safety),
- regulatory agency review,
and clear definitions of - indications, dosing, and target populations.
In practical terms: it’s a promising innovation, but there is still a gap between “reported phase 3 results” and “available in clinical practice.”
What to expect if it becomes available in the future
To set expectations:
Results in alopecia are usually evaluated from 4–6 months, with better clinical assessment at 9–12 months.
There may be initial shedding phases (temporary hair loss) with some hair treatments; that’s why medical follow-up is key to avoid premature discontinuation.
In AGA, realistic goals are usually:
- to stop or slow progression,
- to improve thickness and density,
- and to maintain results with consistent treatment.
Conclusion
Clascoterone 5% is shaping up to be one of the most relevant innovations in androgenetic alopecia because it proposes a different approach: local androgen receptor blockade, with the expectation of reducing systemic effects and expanding options for patients who currently don’t have a comfortable path with oral therapies.
That said, the standard in comprehensive hair medicine remains the same: early diagnosis + personalized plan + follow-up. While evidence continues to evolve and approvals are defined, the best course of action is to maintain medically supported habits and treatments, and avoid self-prescribing.
Practical recommendation
If you are experiencing signs of androgenetic alopecia (receding hairline, crown thinning, diffuse thinning, persistent shedding), the most efficient step is a trichology consultation: clinical evaluation, trichoscopy, differential diagnosis, and development of a comprehensive treatment plan. The earlier you act, the more follicles can be preserved.